Published as: Ivica Klapan et all., Am J Otolaryngol, 2002, 23(1):27-34.
Medical Institutions:
- University Polyclinic Klapan Medical Group, Zagreb
- Department of Otorhinolaryngology and Head & Neck Surgery, Division of Plastic and Reconstructive Head & Neck Surgery and Rhinosinusology, Zagreb University School of Medicine and Zagreb Clinical Hospital Center, Zagreb, Croatia
- Department of Radiology, Zagreb Clinical Hospital Center, Zagreb, Croatia
- Physics Department University of Zagreb, Croatia
- Croatian Society for Telemedicine, Croatian Medical Association, Zagreb, Croatia
- Reference Center for Computer Aided Surgery and Telesurgery, Croatian Ministry of Health, Zagreb, Croatia
- Faculty of Electrical Engineering and Computing, University of Zagreb, Croatia
Address for correspondence:
Ivica Klapan, M.D., Ph.D., University Polyclinic Klapan Medical Group, Ilica 191A, HR-10000 Zagreb, Croatia (poliklinika.klapan@vodatel.com)
Keywords: War wounds, Computer assisted surgery, Three-dimensional visualization, Endoscopy,
This work was in part supported by an unrestrected grant provided by the Ministry of Science and Technology, Republic of Croatia, No. 5-01-543 (Dr. Klapan)
INTRODUCTION
Foreign bodies of paranasal sinuses are quite an infrequent finding. They are usually detected after various types of head trauma. They most commonly occur as a consequence of improper handling firearms or explosives. In the countries at war, e.g., during the Patriotic War in Croatia, adults and children were almost equally exposed to these injuries. This is also the main characteristic of all war injuries.
The presence of metal foreign bodies in the paranasal sinuses may quite frequently be overlooked immediately after injury infliction. The discomforts most commonly reported by patients after trauma include headaches of a varying type and severity, pain in the nose projection and difficult breathing through the nose. These discomforts depend on the entry gunshot wound canal and size of the damaged anatomical field of paranasal sinuses.
The diagnosis should include precise computer tomography (CT) scanning in axial and coronal sections to get an approximate insight into the main characteristics of the gunshot wound canal, foreign body location, and anatomical relationship between the projectile and vital structures of the head (i.e. skull base, carotid artery, optic nerve)1. So, the criteria for the best possible CT image of the paranasal sinus structures are known2. Strictly following these criteria, tissues of different density at these anatomical locations can be differentiated. Neither standard roentgenograms nor lateral tomograms or even CT slices of the highest quality of the region can provide a comprehensive insight into the local finding3. Likewise, endoscopy and/or fiberscopy of the nose will not produce reliable information on the main characteristics of the trauma either, especially if the foreign body is located in the ethmoidal labyrinth or sphenoidal sinus, or if it is in contact with the bony wall of the skull base.
The greatest contribution to the development of rhinosurgical procedures in otorhinolaryngology in the last decade of this millennium has been the implementation of 3D-computer assisted diagnosis and intraoperative navigational techniques, especially in functional endoscopic sinus surgery (FESS). In the region of paranasal sinuses, such an revolutionary approach is of paramount importance for the surgeon because of the proximity of intracranial structures and limited operative field layout hampering spatial orientation during the “standard” operative procedure6,7.
The possibility of exact preoperative, non-invasive visualization of the spatial relationships of anatomic and pathologic structures, including extremely fragile ones11-13, size and extent of pathologic process14-16, and of precisely predicting the course of surgical procedure5, allows the surgeon to achieve considerable advantage in the preoperative examination of the patient and to reduce the risk of intraoperative complications, all this by use of virtual surgery (VS)17 or diagnosis18.
It could be done by using patient’s images created for diagnostic purposes. Storage of the patient's images and diagnoses in a multimedia form in computer systems allows them to be subsequently searched and some specific cases re-examined for analysis and physician education, even via Internet (e.g., Eurorad Project)56-61. By use of DICOM protocol, not only image recordings but all general data of the patient, that have previously been entered onto the diagnostic device console as well as all data on the device setting during patient's image production are transferred from the diagnostic device to computer systems.
From the very beginning of our activities, before the advent of DICOM protocol, image recordings used to be stored on films whereby the image information were partially lost from the diagnostic device. On films, up to 16 levels of the black-and-white image can ideally be distinguished. If images from the films are to be stored in computer systems, the films must be 'scanned', thus partially losing the “black-and-white” contrast on the image, which is then reduced to only 8-10 levels. This leads to additional loss of a substantial part of the data, thus further hampering their interpretation, especially for clinicians on making the diagnosis.
We observed that the level setting and window width observed on the images could not be subsequently changed. Also, the level setting and window width observed on the video recording-images, which allows acceptance of a maximum of 256 different image levels already stored in the computer system cannot be changed.
Finally, the expected contribution of the mentioned computer assisted surgical techniques manifests in defining the most appropriate mode of CT scanning of the head to design the 3D operating field model, and the most appropriate transfer of CT data to and their processing by the computer. In addition, using this approach, the possibility of active and dynamic 3D visualization of the desired anatomical regions is realized8. In this way, 3D reconstruction of anatomic units becomes a routine preoperative procedure8,9,64, providing a highly useful and informative visualization of the regions of interest64, thus bringing advancement in defining the geometric information on anatomical contours of 3D model by the transfer of so-called image pixel to contour pixel5,64. The possibility of data analysis and storage in the 3D form and development of 3D centers at clinical institutions should provide a new quality in proper training of future surgeons.
Concerning biomedical and biotechnical characteristics of our three-dimensional computer assisted FESS project (3D C-FESS), as a fundamental activity of the Expert Center for Computer Aided Surgery and Telesurgery of the Ministry of Health, Republic of Croatia, we strongly believe that this approach deserves highest interest29.
MATERIAL AND METHODS
A. Hardware used in 3D C-FESS:
IMAGE DISPLAY: SGI-O2 Workstation, Color 20’ monitor, 1280x1024x75Hz, 232 colors, double buffered (32+32-bit)
COMPUTER:SGI-O2, 128 MB system RAM, CD, 4GB system disk, IRIX 6.3
operating system, 33600 Baud Modem, Fast Ethernet,
PROCESSING POWER: 4.6 SPEC int 95, 5.4 SPEC fp 95
USER INTERFACE: Mechanical mouse, Keyboard, X-wind./MOTIF/Indigo magic
CT or MRI INPUT : Ethernet using DICOM Standard
OTHER: NTSC/PAL S-video output, HP 1100 A Laser Printer.
Endoscopes, standard FESS-instruments, cold-light sources, monitors, endo-micro camera, video recorder, 3D-digitizer
B. Softwares used in 3D C-FESS:
3D Viewnix V1.1 - http://www.mipg.upenn.edu
Elscint OmniPro 2.2 - http://www.elscint.co.il
Analyze AVW - http://www.mayo.edu/bir
T-Vox V1.0 - http://www.ht.com
SGI Showcase V3.4.1 - http://www.sgi.com
Starvision StarMED - http://www.starvision.com
C. CT scanning
Standard CT scans in coronal and transverse sections of 3-mm thickness were performed on a Sytec 2000+ (General Electric). Five-mm transverse CT sections were performed in a plane parallel with the hard palate and the patient in supine position, whereas 3-mm coronal CT sections were performed in a plane perpendicular to the hard palate with the patient in prone position with neck hyperextension.
These CT images were used to design the static and dynamic 3D models of paranasal sinuses. Two-dimensional coronal and transverse sections were compared with 3D models. The static and dynamic 3D models and virtual endoscopy (VE) of the sinuses were used in surgical planning and were available to the surgeon in the operating room throughout the procedure. All CT images obtained were stored on film and in digital form on a magnetic medium (hard disk).
D. 3D C-FESS
The 3D C-FESS procedure performed by use of a 3D-digitizer was based on the following main principles: a) design of the static and interactive dynamic 3D models of paranasal sinuses and adjacent anatomical structures per viam special computer programs; b) using rotation and changing observation point, separation and segmentation of various structures, and visualization of various structures in different colors; c) defining the degree of particular structure transparency, exclusion of particular structure visualization from the model, and model magnification and diminution; d) animation of 2D-CT sections of the nose and paranasal sinuses with comparison of standard 2D-CT sections of paranasal sinuses with 3D models of the same region; and e) application of VE technique9, when the computer simulation of the endoscopic procedure has already been done.
E. Case reports:
Case 1
K.Z., a 12-year-old child, was inflicted a gunshot wound in the region of the left eye (May 1994). Status: gunshot wound of the left orbit, injury to the lower eyelid and conjunctiva of the left eye bulb. Massive subretinal, retinal and preretinal hemorrhage. The vitreous diffusely blurred with blood. The child was blinded on the injured eye. Six years after the 3D C-FESS surgery, the status of the left eye is completely normal. The vision is normal bilaterally.
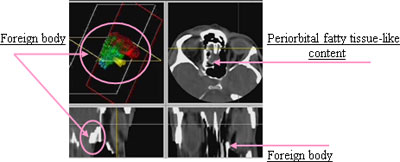
(a) Axial CT images of the hypodense shadow of the metal foreign body, 7-8 mm in size, in the region of posterior cells of the ethmoidal labyrinth, on the left side (Figure 1 a, b, c).
Figure 1 a, b, c. Axial CT-images of the hypodense shadow of the metallic foreign body

The foreign body located adjacently to the medial wall of the orbit, where a discontinuity and discernible fragmented lamina papyracea observed. Local thickening of the medial rectus muscle and a minor hematoma are also seen (CT image not attached). This local finding corresponds to the gunshot wound canal projection. Shadowing of the posterior ethmoidal cells suggests the existence of a more dense, periorbital fatty tissue-like content, which was verified on operation. Anatomical projection of the optic nerve, sphenoidal sinus and right side of the ethmoidal labyrinth were normal, with normal sinus aeration, transparent cellules and intact intracellular septa.
(b) Coronal CT image showing the foreign body position in relation to the medial wall of the orbit, ethmoidal cribriform plate and base of the anterior fontanelle (Figure 2 a, b).
.
Figure 2 a, b.

Foreign body
Using the static 3D model elaborated from 2D CT sinus section, we obtained relative relationships of the borderline areas that are important for the diagnosis of pathologic conditions in the region, which proved to be a significant improvement in comparison with 2D visualization in the form of stratified images (Fig. 3 a,b,c).
Figure 3 a, b, c. Different 3D models with evidence of the metallic foreign body

The route of the endoscope was “simulated” preoperatively. Overlying the respective region onto the volume rendered model with video image, we were able to create various complex anatomical structures, which allowed a highly precise diagnosis as well as the most sophisticated quidance through the operation itself (Figure 4).
Figure 4 a,b,c,d. 2D sagittal-CT and 3D-view of the foreign body
The duration of the operation, done per viam 3D C-FESS technique, was approximately 15 minutes. The main problems, discussed very briefly prior to the operation, were resolved successfully during the operation, is follows: a) the fragmented lamina papyracea observed, b) partial removal of the periorbital fatty tissue-like content from the anterior and posterior ethmoidal cells, which did not allow complete orientation in the surgical field, c) completely normal status of the cribriform plate, bony canal of the optic nerve, and skull base margins.
Case 2
A 28-year-old healthy man suffered a penetrating injury in the region of the left palpebral fissure with a metallic object particle, which caused a 3-mm laceration of the eyelid edge and eyeball penetration involving the entire cornea diameter and continuing into the orbit by 4 mm3. The foreign body was almost completely retained in the orbit, with a minor segment protruding to the region of posterior ethmoid sinus cells.
Orbit x-ray indicated a foreign body, showing a shadow intensity characteristic of a metal object in the region of medial and posterior segments of the orbit, with suspected fracture of the base of the orbit. CT scanning of the orbit revealed a foreign body, 10x30 mm in size, in the cribriform lamina region of the left orbit (Figure 5) .
Figure 5. Coronal, axial and sagittal CT images of the orbit and paranasal sinuses
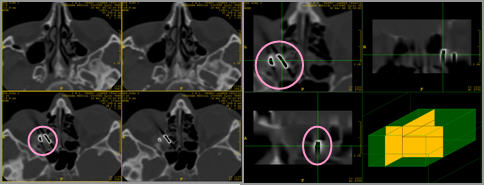
Foreign body partially protruded into the posterior ethmoidal cells, and partially into the orbit, causing dislocation and compression of the muscle rectus medialis and muscle rectus inferior. Other muscles and the optic nerve were intact3. Pronounced chronic inflammatory changes with signs of ostiomeatal block were observed in the region of ethmoidal cells and left maxillary sinus (Figure 6 a,b,c).
Figure 6 a, b, c. Different 3D models of patients head, with evidence of foreign body
Fragmented lamina papyracea

With the use of computer techniques of segmentation and presentation of various tissues with different colors as dynamic 3D model, we enabled visualization of various anatomical structures in real time as well as of their spatial interactive relationships from all aspects possible. Finally, using the technique of VE, we simulated the endoscope tip penetration through the orbit, nose and paranasal sinuses which cannot be explored by the existing endoscopic methods, i.e. using only FESS approach (Fig. 7).
Figure 7. Step-by-step visualization of foreign body per viam VE. 2D-CT and 3D view of volume rendered isolated metallic retrobulbar foreign body

During the 3D C-FESS operation, our main concern was to prevent any additional damage to the muscle rectus medialis, muscle rectus inferior and optic nerve on foreign body removal (Figure 8). As the proximal part of the double-bent tin fragment leaned against the muscle rectus medialis, encircling it by its anterior bent edge along the medial wall of the orbit in parallel with the other bent edge, the act of extirpation had to be carried out in such a way as to slightly rotate the foreign body on its axis and drag it through the region of posterior ethmoids to the nasal region3. Close contact of the distal part of the foreign body with the optic nerve posed an additional problem. On rotating, utmost care was taken not to move the distal part of the foreign body even by a millimeter, to prevent damage to the optic nerve3.
Figure 8. Metallic foreign body after 3D C-FESS removal from the orbit

Case 3.: Metallic foreign body in the right sphenoidal sinus
During the war, the patient suffered a penetrating injury by a shell splinter throughout the ethmoidal labyrinth and sphenoidal sinus. Before the 3D C-FESS treatment, the patient was operated on per viam FESS on three ocasions, without success.
Axial CT scan demonstrated normally ventilated maxillary and sphenoidal sinuses. The mucosa of the right and frontal sinus is thickened. The metallic foreign body is shown in the part of the sphenoidal sinus surrounded by thickened mucosa on the right. Multiple fractures and thickened mucosa within the ethmoidal cells are also seen.
On direct coronal CT scan, the metallic foreign body is seen on the top of the frontal part of the sphenoidal sinus (magnified detail from Fig. b). Computerized reconstruction of the metallic foreign body in coronal view. A different shape of the same metallic foreign body can be noticed.
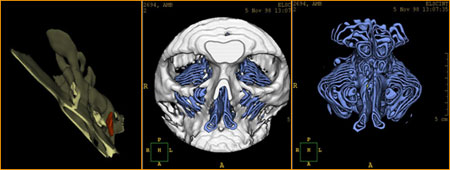
Figure 9 a,b,c,d. Axial CT images of the hypodense shadow of the metallic foreign body in the sphenoidal sinus

Figure 10 a,b. Coronal CT images of the hypodense shadow of the metallic foreign body in the sphenoidal sinus

Figure 11 a,b,c. Sagittal CT images of the hypodense shadow of the metallic foreign body in the sphenoidal sinus

Figure 12 a, b,c,d,e. Different 3D models with evidence of the metallic foreign body

Case 4.: 3D visualization of the metallic foreign body between the maxillary sinus and retromaxillary fossa.
During the war, the patient was injured by a surface-to-air projectile splinter that penetrated through his facial structures. The metallic foreign body was retained in the maxillary sinus, in the borderline area toward the retromaxillary fossa.
Coronal CT scan shows a metallic foreign body within the left maxillary sinus. near the medial wall. The lateral wall of the sinus is completely destroyed. The huge ethmoidal bulla, ethmoidal cells and right maxillary sinus are normally ventilated. The conchal cavities show no abnormalities. The septum is deviated. On horizontal CT scan, the large oval metallic foreign body is seen within the left maxillary sinus.
Figure 13. CT images of the hypodense shadow of the metallic foreign body in the right maxillary sinus

Figure 14. Comparison between 2D-CT and 3D views of the metallic foreign body

DISCUSSION
Is it necessary to remove an asymptomatic foreign body from the paranasal sinuses?
With time, such a permanent local irritant will probably cause chronic irritation of the mucosa, thus leading to its irreversible alterations and causing additional problems, even cancer, as already reported in the literature9,10,. This should be considered a reason enough for surgical treatment, as we have discussed previously1.
The external, classical surgical approach to opening the ethmoid or sphenoid is associated with additional trauma to the as yet intact structures. Therefore, the development of precise instrumentarium has recently made the use of FESS preferable. This surgical approach is the method of choice, not only for a significantly less trauma and time-saving procedure, but also for a reduced hospitalization required. It allows access to anatomical regions of the head that previously could not be reached in this way, so that lesions used to be considered almost inoperable (e.g., foreign body in the projection of the skull base, rhinoliquorrhea, fracture of the bony canal of the optic nerve), can now be successfully treated.
At present, every physician (scientist and clinician) using computer for diagnostic (e.g., radiology) and therapeutic (e.g., surgery) purposes should know that images are processed by use of graphic and computer systems as well as by specialized program systems, in order to better present the anatomy of a particular part of the body with identified diseased areas7,8,11,12,14,17-20.
During the Patriotic War, we were faced with many war injuries of the head and neck including the evidence of metallic foreign bodies in the region of paranasal sinuses19. Although we used the FESS approach, sometimes we were unable to finish the operation successfully. Performing our own 3D-approach in computer assisted functional endoscopic sinus surgery (3D C-FESS) we were able to “look inside” the patient during surgical planning as well as at the time of surgery.
Owing to the development of highly sophisticated technologies of the 21st century, first of all informatic sciences, a specific approach in the surgery of FESS has also been developed, including computer-assisted operations in third dimension (3D C-FESS), which offer the possibility of dynamic intraoperative examination of the 3D projection of the head, as well as preoperative computer-assisted determination of operability of the anatomical regions of the head.
Such a 3D C-FESS approach, being developed by the Šalata-Zagreb ENT rhinosurgical team since the, early 90s, has already shown a number of advantages in the surgery of paranasal sinuses.
With the use of 3D model, our orientation in the operative field is considerably facilitated20-21 (see case reports 1-4), and all procedures and manipulations are performed with greater certainty and safety22-23. Subsequent computer analysis of digital CT or MRI image information, translating them from two-dimensional (2D) into the 3D form, allows for a reliable diagnosis to make20 (Figure 7), especially on defining precise localization and spread of the pathologic process14 (Figure 12). The possibility of isolated and selective visualization of particular tissues and structures within the model, including distinct differentiation of the borderline even between two different soft tissue structures (e.g., normal mucosa and tumor)14, in spite of some contradictory reports24, provides additional diagnostic information on the relationship between the pathologic process and the surrounding anatomic areas. Separate models of bones, healthy tissue, affected tissue, air space of paranasal sinuses (Figure 15), and of all significant anatomic entities of the operative field, have been developed.
Figure 15 a,b,c. 3D view of extrapolated empty air space of the paranasal sinuses (different models for different purposes)
Multiple series of images can be simultaneously observed in different color tables and at various magnification, with various grades of transparency, observing them as a unique 3D model system.
The more so, various angles of imaging, visualization of the superficial anatomy, selective visualization of the tumor and vasculature, simulaton of surgical procedures, measurement of the size of anatomic areas, selective 3D model staining, delineation, 3D rotation, different views, shifts, cuts, separations, labeling, and animation, are only some of the numerous possibilities used in our preoperative planning, intraoperative computer guidance (Figure 16), and postoperative analysis.
Figure 16. Computer aided surgery: removal of the foreign body per viam 3D-CAS

During the operative procedure, the computer with its operative field image allowed us, by means of up-to-date technologies, to connect the operative instrumentarium to spatial digitalizers connected to the computer. Upon the completion of the operation, we compared the preoperative and postoperative images and models of the operative field, and studied video records of the procedure itself. Using intraoperative records, animated images of the real procedure performed can be designed, which we did on many occasions (URL:http://salata.mef.hr/3D-CFESS, case report: Metallic retrobulbar foreign body). By means of computer records labeled coordinate shifts of 3D digitalizer during the surgery, an animated image of the course of operation in the form of journey, i.e. operative field fly-through in the real patient, can be designed. Beside otorhinolaryngology8,14,17-20, this has also been used in other fields10. The more so, in addition to educational applications, VS has offered us the possibility of preoperative planning in sinus surgery, and has become a very important segment in surgical training and planning of each individual surgical intervention.
In the activities of our 3D C-FESS team, these analyses are becoming routine
procedures, as well as in other ENT centers elsewhere4,5,18,25, for oral, maxillofacial and plastic surgery (Figure 17).
Figure 17. Preoperative planning in the surgery of the nose and paranasal sinuses. Case report: foreign body in the sphenoidal sinus.

The three-dimensional model completely presents the relative relations of borderline areas that are of utmost diagnostic importance, which is a considerable advancement compared with standard 2D stratified imaging.
The complex software systems allow visualization of a CT or MRI section in its natural course (the course of examination performed), or in an imaginary, arbitrary course. Particular images can be transferred, processed and deleted, or can be presented in animated images. The series of images can be changed, or images can be generated in different projections through the volume recorded.
Before the development of 3D spatial model, each individual image or a series of images have to be segmented, in order to single out the image parts of interest.
Comparative analysis of 3D anatomic models with intraoperative finding shows the 3D volume rendering image to be very good, actually a visualization standard that allows imaging likewise the real intraoperative anatomy6,53,64 (Figure 7g vs Figure 8).
The technique of examination intended to realize in the proposed study provides, according to many authors, optimal visualization of the paranasal sinus anatomy. Moreover, by use of this approach, some substantial advancements are achieved in the diagnosis of the pathologic state of paranasal sinuses, based on CT analysis, e.g. (a) basic CT diagnostics has become an important aid in the diagnosis of chronic sinusitis, in terms of the follow-up and prognosis of the course and treatment outcome52; (b) additional axial or coronal sections are avoided by the development and use of 3D model (so-called volume-rendering technique) for diagnostic purposes; (c) as indicated in (b), the dose of irradiation to which the patient is exposed is considerably reduced by the use of volume rendering technique; etc.
The potential commentary on patient selection on the basis of limited coronal CT scan actually refers to a well known term. The aim of such an examination is to reduce the dose of irradiation to which the patient is exposed (primarily eye lens), with the highest diagnostic benefit. Layer thickness, shift, gantry, and window are internationally standardized and accepted values, thus being reproducible all over the world. DICOM protocol56,69,70 is an internationally adopted transfer (networking) standard to link medical instruments (CT, US, x-ray) and personal computer (PC) or graphic workstation.The software for 3D modeling is included in the line of many programming companies all over the world, and is based on the same principles aiming at combining and processing of digitalized data from a medical diagnostic device to obtain a three-dimensional picture or image of a precisely defined structure.
Therefore, we do declare that the method is standardized, reproducible and distinctly defined49,50,52, and it is by no means contradictory. The method is available to any clinician using CT devices with DICOM protocol in his practice. Then, a software type that meets our needs and conditions must be chosen. Occasionally, only a computer system of specific properties56,64, e.g., the size of working memory and disk subsystem, rate and ability of graphic subsystem, has to be chosen.
With defining the procedure of the use of advanced techniques of computer analysis of image data, the 3D method of visualization represents a significant scientific contribution which has also been demonstrated to be of immediate practical value.
Finally, renowned authorities in the fields of radiology60,61,64 and otorhinolaryngology8,14,17,18,36,62, who initiated the development of computer assisted diagnosis and surgery (CAS) as early as the early '80s, have among others defined indications for CAS in the field of ENT. This is primarily the region of paranasal sinuses11,18-20,35,36,62,63, especially in case of narrow and obstructed (difficult) frontal recessus54 and when there is a need of frontal sinus drainage17,62,63, with so-called dangerously laid ethmoidal roof, collapsed cribriform lamina, etc.
The advances in minimally invasive surgery imply great benefits for the patients. However, we are fully aware of the fact that even the most skilful surgeons have reached limits of their skill in ever more demanding operations. A new step in the development of these activities is the use of robotized surgery21-25,53 and Tele-3D-computer assisted surgery26-33, as well as Internet applications of diagnostic (e.g., radiology)56-61 and surgical techniques29.
LITERATURE
1. Mladina R, Hat J, Klapan I, Heinzel B. An endoscopic approach to metallic foreign bodies of the nose and paranasal sinuses. Am J Otolaryngol 16:276-279, 1995.
2. Zienrich SJ, Kennedy DW, Rosenbaum AE. CT of nasal cavity and paranasal sinuses: Images requirements for functional endoscopic sinus surgery. J Radiol 1987; 163:769-775
3. Klapan I, Šimičić Lj, Rišavi R, Bešenski N, Bumber Ž, Štiglmayer N, Janjanin S. Dynamic 3D computer-assisted reconstruction of metallic retrobulbar foreign body for diagnostic and surgical purposes. Case report: orbital injury with ethmoid bone involvement. Orbit 2000 (submitted)
4. Klimek L, Mosges M, Schlondorff G, Mann W. Development of computer-aided surgery for otorhinolaryngology. Comput Aided Surg 3:194-201, 1998.
5. Mann W, Klimek L. Indications for computer-assisted surgery in otorhinolaryngology. Comput Aided Surg 3:202-204, 1998.
6. Anon J, Klimek L, Mosges R, Zienrich SJ. Computer-assisted endoscopic sinus surgery. Otolaryngol Clin North Am 30:389-401, 1997.
7. Gunkel AR, Freysinger W, Martin A, Volklein C, Bale RJ, Vogele M, Thumfart WF. 3D image guided endonasal surgery with a microdebrider. Laryngoscope 107:834-838, 1997.
8. Šimičić Lj, Klapan I, Simović S, Brzović Z, Vukoja M, Rišavi R, Gortan D. Computer assisted functional endoscopic sinus surgery. Video texture mapping of 3D models. E.R.S. and I.S.I.A.N. Meeting, Wienna, Austria, (H. Stammberger, G. Wolf), Monduzzi Editore, Bologna, pp. 281-285, 1998.
9. Birnmeyer G. Uber spatfolgen metallischer fremdkorper der nasennebenhohlen. Z Laryngol Rhinol Otol 42:778-785, 1963.
10. Acheson ED, Pippard EC, Winter PD. Nasal carcinoma in the Northamptonshire boot and shoe industry: Is it declining? Br J Cancer 46:940, 1982.
11. Hauser R, Westermann B, Probst R. Non.invasive 3D patient registration for image
guided intranasal surgery. Medical Robotics Comput Assisted Surg, New York, Springer, str. 327-336, 1997.
12. Vannier MW, Marsh JL. 3D imaging, surgical planning and image guided therapy. Radiol
Clin North Am 34:545-563, 1996.
13. Vinas FC, Zamorano L, Buciuc R, QH L, Shamsa F. Application accuracy study of a semipermanentm fiducial system for frameless stereotaxis. Comput Aided Surg 2:257-263, 1997.
14. Elolf E, Tatagiba M, Samii M. 3D-computer tomographic reconstruction: planning tool for surgery of skull base pathologies. Comput Aided Surg 3:89-94, 1998.
15. Elolf E, Tatagiba M, Samii M. Colorcodes 3D-CT for pathologies in and around the petrous bone. Klin Neuroradiol 7:72-76, 1997.
16. Burtscher J, Kremser C, Seiwald M, Obwegeser A, Wagner M, Aichner F,
Twerdy K, Felber S. 3D-computer assisted MRI for neurosurgical planning in parasagittal and parafalcine central region tumors. Comput Aided Surg 3:27-32, 1998.
17. Holtel MR, Burgess LP, Jones SB. Virtual realiry and technologic solutions in
Otolaryngology. Otolaryngol Head Neck Surg 121(2):181, 1999.
18. Vrabec JT, Johnson RF, Guinto FC. 3D-virtual endoscopy of the temporal bone.
Otolaryngol Head Neck Surg 121(2):225, 1999.
19. Klapan I, Šimičić Lj, Kubat M, Rišavi R. Fracture of the ethmoid and medial
orbital wall. Removal of the bullet per viam 3D C-FESS technique, 3rdEUFOS (ed. Ribari O, Hirschberg A), Monduzzi Editore, Bologna, pp. 83-87, vol. II, 1996.
20. Burtscher J, Kremser C, Seiwald M, Obwegeser A, Wagner M, Aichner F, Twerdy K, Felber S. 3D-computer assisted MRI for neurosurgical planning in parasagittal and parafalcine central region tumors. Comput Aided Surg 3:27-32, 1998.
21. Santler G, Karcher H, Gaggl A, Kern R. Stereolithography versus 3D models:
comparison of production method, indication and accuracy. Comp Aided Surg 3: 248-256, 1998.
22. Martel AL, Heid O, Slomczykowski M. Assessment of 3D MRI fast low angle shot images for computer assisted spinal surgery. Comput Aided Surg 3:40-44, 1998.
23. Olson G, Citardi M. Image-guided functional Endoscopic sinus surgery. Otolaryngol Head Neck Surg 121(2):187, 1999.
24. Mitchell AO, Alburger JF, Bolger WE, Frew MI, Richardson AC. Three dimensional imaging of the pterygopalatine fossa. Otolaryngol Head Neck Surg 121(2):128, 1999.
25. Hardenack M, Bucher N, Falk A, Harders A. Preoperative planning and intraoperative navigation: status quo and perspectives. Comput Aided Surg 3:153-158, 1998.
26. Ecke U, Klimek L, Muller W, Ziegler R, Mann W. Virtual reality: preparation and
execution of sinus surgery. Comput Aided Surg 3:45-50, 1998.
27. Hassfeld S, Muhling J. Navigation in maxillofacial and craniofacial surgery. Comput Aided Surg 3:183-187, 1998.
28. Klapan I, Šimičić Lj. www.mef.hr/MODERNRHINOLOGY













